The Nurse Of Royal Free Hospital, London says: Severe patients of COVID-19 can get a life if they get a ventilator. With the help of ventilators, they can be pulled out of the mouth of death.
When patients are unable to take oxygen by themselves, it is possible to transport oxygen to the patient’s lungs with the help of a ventilator and remove carbon dioxide.
But it is not possible to save the corona patient only with the help of a ventilator. This is the reason why teams of medical professionals around the world have to make some tough decisions, including removing respirators in case a patient is not better.
Juanita Nitla, chief nurse of the Intensive Care Unit (ICU) of the Royal Free Hospital, London, told the BBC, “It is excruciating to switch off the ventilator. Sometimes I feel that I am responsible for someone’s death.” “
Born in South India, Nita has been working as an Intensive Care Specialist Nurse in the National Health Service of England for the past 16 years. “Turning off the ventilator is also part of my job,” the 42-year-old told the BBC.
The Nurse Of Royal Free Hospital, London says: “I take life to save lives”

Dying wish
In the second week of April, Nitla arrived at her work in the morning shift on a busy morning, according to the ICU register, she had to stop treating a COVID-19 patient.
The patient was a community health nurse whose age was more than 50 years. Nitla informed the patient’s daughter about this procedure.
Nitla said, “I told her that her mother is in no pain. She is in a state of rest. I also asked her about her mother’s wishes and religious beliefs.
The ICU has beds one by one. There were other patients who were unconscious around Nitla’s seriously ill patient.

Nitla said, “The nurse was where eight beds were placed. All the patients were seriously ill. I dropped the curtain and set off all the alarms.”
The entire medical team stayed as if for a few moments. “The nurses stopped talking among themselves. The dignity and convenience of the patients is our priority,” said Nitla.
Nitla then placed the phone near the patient’s ear and asked her daughter to speak. About this phone call, Nitla said, “For me, it was just a phone call, but it is very important for the family. They wanted to make a video call, but unfortunately, it is allowed to carry mobile phones Switch off inside the ICU does not happen. “
As per the request of the patient’s family, Nitla played an exclusive music video from the computer. After this, Nitla switched off to turn off the ventilator.

“I sit next to him, holding his hand till his death,” said Nitla.
The medical team takes the decision very carefully to help with breathing and to stop treatment.
In this, the age, health status of the patient, effect of treatment, and hope of recovery are taken into consideration. The patient was killed within five minutes of shutting down the ventilator support of Nitla.
Nitla said, “I was watching the flashing light on the monitor, the flat line started appearing on the screen after the heart rate was zero.”
Die alone
Nitla then separated the tubes delivering the medicine from the body. The daughter of these most unknown patients was being talked over the phone continuously.
She was also praying on the phone. With a burden on his heart, Nitla lifted the handset and told the patient’s daughter that everything was over.
But the duty of nurse Nitla does not end with the death of the patient. She told the BBC, “With a colleague, I bathed them on the bed and wrapped them in a white shroud. Then put their bodies in body bags. I made a cross mark on their forehead before closing the bag.”
In the time before the coronavirus, relatives used to talk face to face to stop treatment. Before turning off the life support system, close relatives were also allowed to enter the ICU.
But this is not happening in most parts of the world. Nitla sees such patients, also tries to help them to recover from this infection.
She says, “It is sad to see someone die alone like this.”Nitla sees patients struggling and yearning to breathe and it is also very stressful to see.
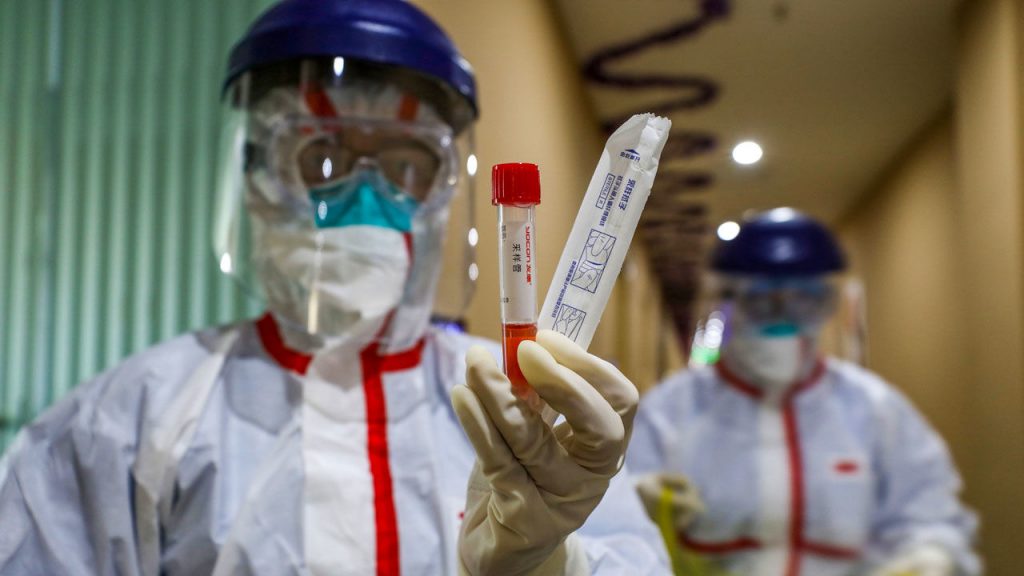
No beds in hospital
Due to an increase in the number of patients in the hospital, the space of 34 beds in the critical care unit of the hospital has been increased to 60 beds. There are patients on all beds.
A team of 175 nurses are working day and night to look after the ICU patients. “We usually average one nurse per patient in a critical care unit.
But now the average is one nurse per three patients. A nurse will have to be deployed for every six patients as the situation worsens,” says Nitla.
Symptoms of corona have appeared in some nurses of Nitla’s team, after which those people have been sent to self-isolation. The hospital has also started training other nurses to work in critical care.
“We shake hands before Shift starts and call each other Stay Safe. We keep an eye on each other. We want to make sure that all of us have gloves, masks, and protective gear,” explains Nitla. Or not. “
There is a shortage of ventilators, infusion pumps, oxygen cylinders, and many medicines in the hospital, but there is a Personal Protection Equipment (PPE) kits for the entire team.
Nitla’s ICU is dying every day, and this was not the case before the corona infection.

“It is like breaking courage,” says Nitla.
Being a head nurse, Nitla sometimes has to suppress her fears. Nitla said, “I have nightmares. I can’t sleep. I worry that I have not been infected myself. I talk to colleagues, everyone is scared.”
Last year, Nitla was away from work for several months due to TB disease. She knows that her lung capacity is not the same. Nitla said, “I should not work, people say so. But there is a situation of the epidemic.
I am leaving everything and doing my work. After the Shift is complete, I think about the patients whose death to take care of me. During this time, but after getting out of the hospital, I try to forget these things. “
American war of Independence: Everything the USA has made wrong – and got right
Table of Contents







Add Comment